
Diagnosis
Radiology
A chest X-ray is taken of the posterior-anterior chest. Physicians are looking for the lobal consolidation resulting from calcification and inflammation 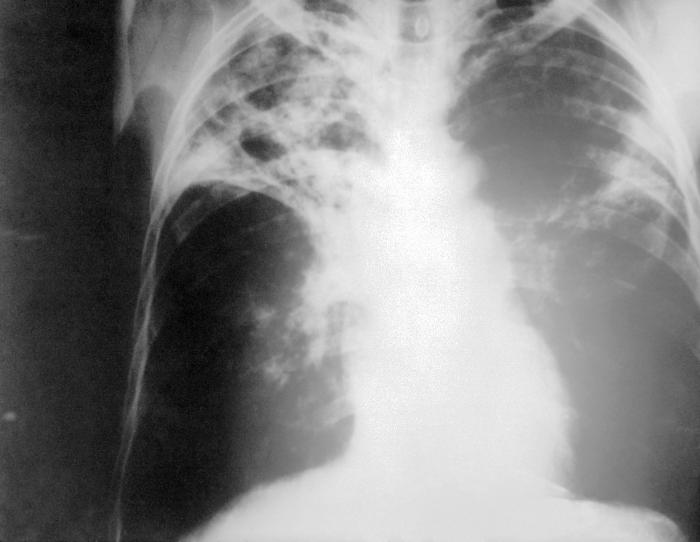 within the lung parenchyma. The presence of hilar lymphadenopathy is a hallmark sign for the presence of pulmonary TB as well as pleural effusion caused from disease manifestation. The disadvantages of using this method to diagnosis TB are that the appearance of the film appears atypical, almost like normal, for an immunosuppressed patient (e.g. HIV). Furthermore, one cannot distinguish between old and active disease; or even make a definitive diagnosis of what is causing irregularities on the film. As a result, this test is normally used in conjunction with a culture test.
within the lung parenchyma. The presence of hilar lymphadenopathy is a hallmark sign for the presence of pulmonary TB as well as pleural effusion caused from disease manifestation. The disadvantages of using this method to diagnosis TB are that the appearance of the film appears atypical, almost like normal, for an immunosuppressed patient (e.g. HIV). Furthermore, one cannot distinguish between old and active disease; or even make a definitive diagnosis of what is causing irregularities on the film. As a result, this test is normally used in conjunction with a culture test.
"Tuberculosis X-ray" image courtesy of Wikimedia Commons under Creative Commons License: Original image
Sputum microscopy and culture
A test involving sputum microscopy is used specifically to aid diagnosis for active pulmonary TB. Firstly, sputum samples of the patient are taken and placed onto slides which are then prepared for viewing using one of two typical methods; either fluorescence microscopy or Ziehl-Neelson staining. The latter is the more conventional method utilising a combination of cabol fuchsin, hydrochloric acid and methylene blue to stain any present acid-fast bacilli bright red. On the other hand, an auramine-rhodamine stain can be applied which causes acid-fast bacilli to display a red-yellow fluorescence and is the more sensitive of the two methods even though it is not specific for the TB pathogens.
Definitive diagnosis for TB ultimately relies on culture tests for the presence of active bacteria. Samples of sputum or a biopsy (in cases of non-pulmonary TB) are grown on plates and tested for the presence of specific strains of the pathogen. Furthermore, although this is very important test both microscopy and culture are expensive, they require special equipment and trained technicians and more unfortunately they take a long time to obtain results. The contagious nature of TB means the patient is capable of spreading the pathogen before they have even been accurately diagnosed and processed for a treatment plan.
Tuberculin skin tests (TST)
These tests can provide evidence for the exposure of a patient to the bacteria causing TB and there many variations of it, including the Heaf test and the Mantoux test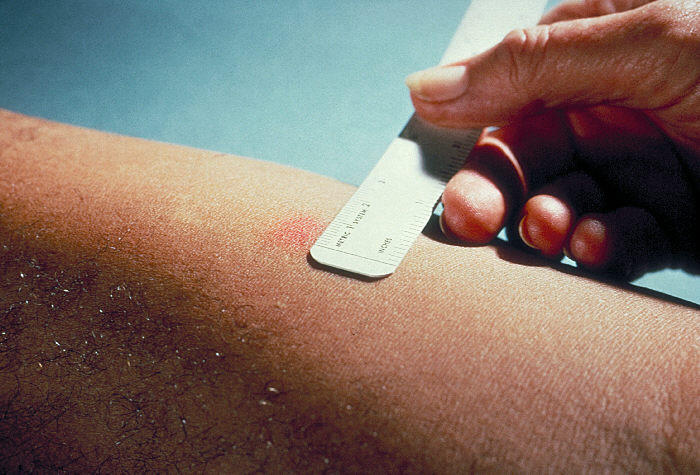 which is the more desired method used today.
which is the more desired method used today.
The Mantoux test involves injecting a patient with a tuberculin preparation and then waiting up to 72 hours to observe any change in the skin tone. A patient who has been exposed to the pathogen will be expected to mount an immune response to the tuberculin and therefore this can be seen as a inflamed mark on the skin. The reaction, if any, is read by measuring the diameter of the inflamed area:
- A diameter less than 6mm is considered a negative result and therefore this patient may be eligible to have the BCG vaccination. However, physicians must be wary of false-negatives in the results which can be caused by HIV sufferers.
- An observed diameter of 6-15mm indicates that the patient has previously had the BCG vaccination, previously had TB or has been in contact with an environmental mycobacterium not associated with the disease.
- A reaction creating a diameter greater than 15mm strongly suggests the patient may be infected and further diagnostic tests should follow.
"Mantoux test" image courtesy of Wikimedia Commons under Creative Commons License: Original image
Improving the diagnostic system
As discussed above, TST's are used extensively to aid diagnosis of TB or link a patient to previous exposure. However, there have been many issues relating to the accuracy of interpreting the results, such as, the BCG vaccine which can cause false-positives. A relatively new test has been introduced, called QuantiFERON®-TB Gold, which removes the vaccination issue. It is a laboratory based test involving a sample of the patients blood which are mixed with antigens, ESAT-6 and CFP-10, and trigger an immune response from the white blood cells. Patients who are infected with Mycobacterium TB have lymphocytes that recognize these antigens in a process that involves the secretion of interferon-γ (IFN-γ); it is this molecule that is detected for a positive result.
The QuantiFERON®-TB Gold test does not distinguish between latent or active TB, however possesses many advantages, including;
- The results can be obtained as soon as the blood sample is taken
- The test only requires one patient visit unlike the TST's
- The antigens used are absent from all BCG strains to prevent interference
So what is wrong with the test? Well, so far the performance of the test has not been researched enough relating to immunocompromised patients(HIV-positive) which will cause a decrease in the amount of IFN-γ. In addition, there are some strains of mycobacterium (M. kansasii, M. szulgai or M. marinum) that contain the antigens used and therefore will cause false-positive results. Finally, the results must be processed within 12 hours of taking the blood sample; a problem in certain areas where the laboratories are a great distance away.